Tag: Alzheimer’s
High Copper Symptoms: A Second Opinion on Anxiety, Dumping Episodes & How to Test for High Copper
SECOND OPINION SERIES High Copper Symptoms and the Biochemical Cause Copper plays essential roles in [...]
2 Comments
Raising Ceruloplasmin to Improve Copper Overload Symptoms
How to Increase Ceruloplasmin Naturally: Understanding Copper Balance, Free Copper, and Mental Health If you’re [...]
Methylene Blue: A Promising Treatment for Mitochondrial Dysfunction
Methylene Blue: A Potential Treatment for Depression, Alzheimer’s, Parkinson’s, and Other Neurological Disorders Methylene Blue [...]
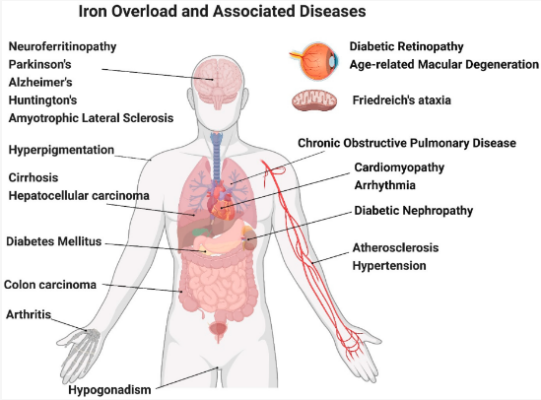
Ferritin Testing: Iron Toxicity and its Links to Oxidative Stress, Gut Health, and Age Related Disease
Iron Overload: Ferritin, Toxic Overload, Liver Inflammation and Brain Health Iron, a critical mineral, is [...]
Alzheimer’s and MT Promoter Therapy
Notes from a physician workshop given by Dr William Walsh, Phd., 2016 Treatment of Alzheimer’s [...]
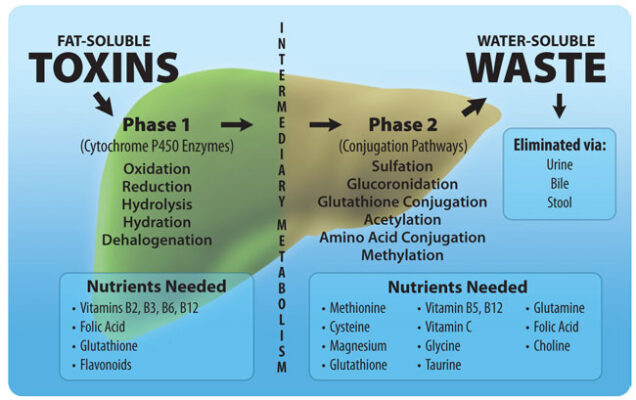
Toxic Overload, Depression and Detoxification Pathways
Toxic Overload and Depression: The Effect of Toxins on Methylation and Glutathione Depletion This article [...]
Alzheimer’s – Dale Bredesen MD; Cognoscopy Lab Test Panel
Understanding the Bredesen Protocol: A Holistic Approach to Alzheimer’s Disease Prevention and Reversal Receiving a [...]
How to Cure Alzheimer’s; Gundry MD Interviews Dr Dale Bredesen
How To Cure Alzheimer’s Summary of video. What you need to check; what you need [...]
Rhonda Patrick, PhD. Interviews Dale Bredesen MD Alzheimers
This video interviews Dale E. Bredesen, M.D., a neurology professor at the Easton Laboratories for [...]