We are all either undermethylators, overmethylators or normal methylators.
Many persons with depression are under or over methylators. Depressed women during pregnancy are frequently undermethylators. The good news is, there are many foods that provide #methionine to reverse the deficiency and lift depression.
This published study in the Psych Congress Journal suggests that women who have maternal depression and are undermethylated, often give birth to children who experience depression due to their own ensuing condition of #undermethylation.
Whole blood histamine test is a lab that indicates methylation status. An excellent natural therapy may be methionine or SAMe supplements or foods that are high in methionine. If you have high blood histamines you may be undermethylated. Persons with seasonal allergies are frequently undermethylated. I recommend you get your levels tested before indulging in high methionine foods because your depression may in fact be associated with overmethylation, which requires an opposite approach, to lower methionine.
In consideration of the the study below, know your methylation status, particularly if you are depressed, and to combat during pregnancy, eat foods high in methionine and or take supplements. It won’t just make the mother feel better, but improves chance child won’t end up with depression.
Maternal Depression Linked to #dna Methylation Changes in Offspring
by Will Boggs MD, Psych Congress
By Will Boggs MD
Maternal depression is associated with widespread changes in DNA methylation in their offspring that may persist into adulthood, researchers from Canada report.
“These data further demonstrate the potential long-term consequences of maternal depression for the health of future generations and the importance of mental health and social support of mothers and would be mothers for the physical health of newborn and children,” Dr. Moshe Szyf from McGill University in Montreal, Quebec, told Reuters Health by email. “What is remarkable is that the mental state of a mother causes changes in DNA methylation in the newborns in the immune system, not just the brain.”
Maternal mood disorders and stress during pregnancy can result in attention learning deficits during childhood and mood disorders during adulthood for their offspring. Evidence suggests these consequences may be mediated by modifications of DNA methylation levels.
Dr. Szyf’s team investigated possible associations between maternal depression and DNA methylation changes in T lymphocytes from neonatal cord blood and in hippocampal brain tissues from adults with or without histories of maternal depression.
Offspring of depressed mothers, however, showed significant differences in DNA methylation from those of nondepressed mothers in 145 T lymphocyte CG sites. Most (75.5%) were hypomethylated in the maternal depression group compared with the control group.
“One of the main surprises was that we found a larger effect of maternal depression on the babies’ DNA methylation than the maternal DNA methylation,” Dr. Szyf said. “The second surprise was that it seems that the effect is a consequence of lifelong depression rather than depression only around the pregnancy period.”
“For healthy babies to develop into healthy adults it is important to have healthy mothers,” Dr. Szyf said. “And this involves not only physical and metabolic health but also mental and social wellbeing. This hopefully will be an important pillar in prenatal care as well as public policy relating to preconception health.”
“The #epigenetic consequences of maternal depression might suggest using epigenetic interventions for prevention and reversal of the impacts of maternal depression on the offspring,” Dr. Szyf added. “One clinical potential of the data is the possibility of developing biomarkers of maternal depression that might serve as predictors of lifelong health risks and guide early interventions.”
Dr. Joanne Ryan from University of Melbourne’s Murdoch Childrens Research Institute, Australia, who recently reviewed #epigenetics and depressive disorders, told Reuters Health by email, “An important next step in this research is to determine whether these methylation differences and associated with health outcomes in the infants/children. Maternal depression during pregnancy has been associated with long-term negative outcomes in the child — the data from this study should be used to determine whether such effects can be mediated by differential DNA methylation.”
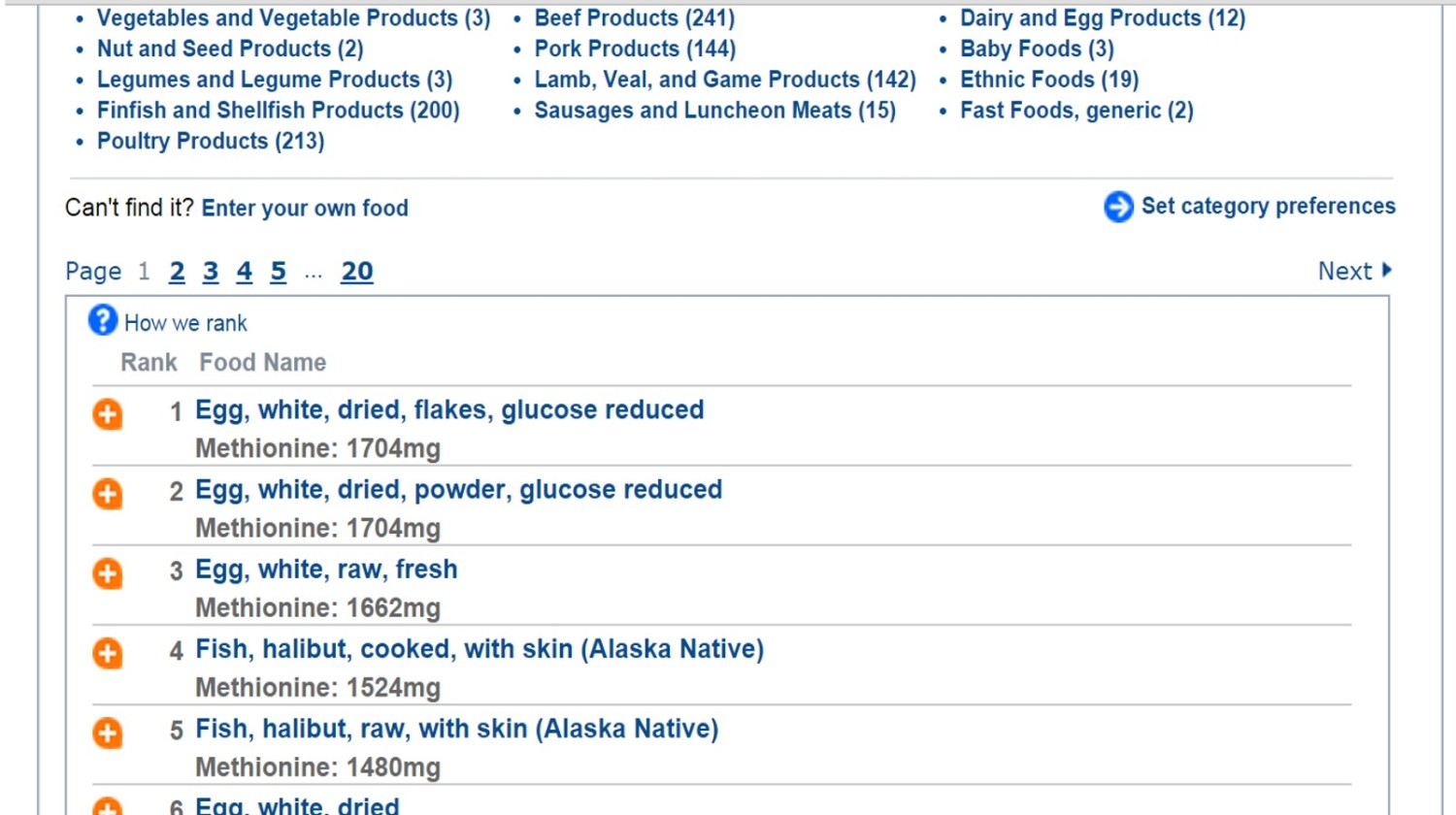
To find out more about good foods during pregnancy to help with low methionine, we checked with our favorite food resource.
https://nutritiondata.self.com/